Uterine Rupture In Pregnancy
Contents:
- Symptoms of a Uterine Rupture
- Reasons
- Diagnostics
- The Treatment of the Uterine Rupture
- Complications and Consequences
- Preventive Measures Against Uterine Rupture
Uterine rupture is a breach of uterine walls integrity during pregnancy and the process of labor. Most often, the rupture occurs on those areas where the tissues of the uterine were changed (on the area where there are cicatrixes left after a surgical operation). However, the rupture may also get to the uterine wall that has been unchanged. The lower part of a uterine is the place that is subject to ruptures in the majority of cases.
This complication that occurs during the course of pregnancy or the process of labor is quite dangerous for the life of a mother and her baby. Therefore, you should start treating it as soon as possible and take preventive measures against it.
Symptoms of a Uterine Rupture
- Discomfort and tension in the lower areas of the belly.
- An acute lancinating pain in the area of the uterine.
- Strangury urination and blood in the urine.
- Labor pains and expulsive pains (the contractions of the uterus that help the baby to be born) being quite painful.
- Bloody discharge from vagina.
- The baby moving actively.
- An appearance of the swelling in the lower part of the belly. The swelling gets bigger and bigger.
- Weak labor process that then, almost absolutely stops. (The expulsive pains do not help the baby to move down).
- Clammy sweat, mucous membranes and skin integument being pale.
- A decrease of the arterial pressure of a mother, barely palpable and frequent pulse.
Reasons
There may be several reasons for a uterine rupture.
There are some obstacles on the way of the baby that do not let him or her move:
The sizes of the fetus and the mother’s pelvis do not match:
- the pelvic ring of a mother may be narrow too much (contracted pelvis) for the baby’s head to get through it;
- the baby being very big (the baby’s weight is more than 4000 g.);
- hydrocephalus of the fetus (the baby’s head gets bigger due to the liquid that accumulates in the skull chamber).
The shoulder presentation of the fetus (The fetus is located so that it is perpendicular to the axis of the neck of the womb).
There is a tumor in the small pelvis.
There is a pathological change of a uterine wall:
- Changes of inflammatory nature. For example, chronic endometritis (the inflammation of the uterine mucous membrane) that usually occurs before pregnancy.
- Changes connected with cicatxes. For example, a cicatrix on the uterus (the wall of the uterus becomes thinner in the areas on which there was a caesarean section carried out or any neoformations were removed (myomatous nods)).
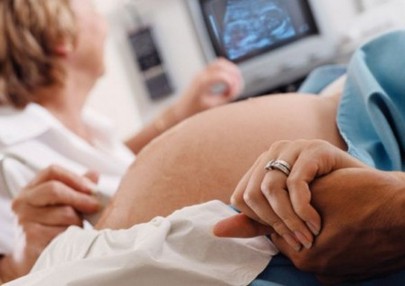
Diagnostics
Analyzing the anamneses of the illness and the patient’s complaints – when (how long does a patient have painful sensations in the lower part of the belly and bloody discharge?) did painful sensations in the lower part of the belly and bloody discharge start to occur? Are the complaints connected with the process of labor or any surgical operations? What is the opinion of the patient as to what may be the reasons for the symptoms?
Analyzing the gynecological and obstetric anamneses – What gynecological illnesses has the patient had? Were there any surgical operations? Former cases of pregnancy and labor (peculiarities and results)? What are the peculiarities of this course of pregnancy?
Objective investigation – the examination of the patient, the measurement of her arterial pressure and pulse, palpation (touching) of the belly and the uterus. External obstetric investigation. A doctor defines the form of the uterus, the location of the baby and the muscle tension of the uterus with the help of his/her hands.
Ultrasound examination of the uterus and the fetus – this method allows to see if there is a case of the muscle layer of the uterus getting thinner in any area, a doctor is also able to see if there are any cicatrixes that appeared after surgical operations and evaluate their condition. Cardiotocography – a method that allows you to evaluate, for sure, the condition of the fetus according to the changes of the cardiovascular system activity indexes.
The use of other methods in the process of diagnostics is limited. Most often, it’s so because you don’t have much time here. You should start treating the uterine rupture as soon as possible. For example, you should discuss with your doctor when it’s possible to carry out a procedure of the caesarean section so that to take the baby out of your body. This procedure, as well, should be done as soon as possible.
The Treatment of the Uterine Rupture
The main aim here is to take the baby out of your body as soon as possible so that to save his or her life. It’s also important to stop the bleeding so that to save the mother.
The main focus of the conservative therapy should be on the following things:
- it’s necessary to stop the bleeding with the help of fibrinolysis inhibitors (these are the agents that influence on the stopping of the natural dissolution of thrombuses (clots of blood);
- it’s necessary to decrease the muscle tension of the uterus with help of muscle relaxants (agents that relax all the muscles) – they are usually part of the narcosis;
- it’s necessary to fight with the consequences of the blood loss (intravenous injection of the colloid and aqueous solutions (low-molecular dextrans – the drugs that are made on the base of derivative starch. They get the water into a vessel opening thus increasing the arterial pressure) – they are used in case of blood transfusion and in order to increase the arterial pressure);
- it’s necessary to take preventive measures against infectious complications. This is done with the help of antibacterial drugs (the drugs that kill or prevent the bacteria from reproducing).
A caesarean section (emergency surgical operation) is always carried out when there is a case of uterine rupture. Once the baby is taken out of the uterus, the rupture is taken in thus, the bleeding is stopped. The uterus is removed only when there is quite a serious case of defects in the uterine walls and there is no way to take them in.
Complications and Consequences

- Acute hypoxia of the fetus (the fetus doesn’t get enough oxygen because there isn’t enough blood supply).
- Prenatal death.
- Hemorrhagic shock (a progressive disorder of the nervous system’s vitally important functions, the disorder of the blood circulation and respiration systems since there is a significant loss of blood).
- The development of disseminated intravascular coagulation symptom (a serious disorder of blood coagulation system because of which intravenous clots of blood and bleedings may occur).
Preventive Measures Against Uterine Rupture
Planning pregnancy and getting ready to it (excluding the possibility of the occurrence of an unwanted pregnancy, detection and treatment of chronic diseases a woman has before the pregnancy occurs). It’s recommended to start planning pregnancy at least two years after the operations on the uterus.
A pregnant woman should register at a maternity hospital on time (before the 12th week of the pregnancy). A woman should visit an obstetrician – gynecologist regularly (once a month during the first trimester, once in 2-3 weeks during the second trimester and once in 7-10 days in the third trimester).
Detecting the Risk Factors of a Uterine Rupture Beforehand
An ultrasound investigation will help you keep a watchful eye on the cicatrix you have on your uterus. Starting from the 20th – 22nd week of pregnancy you should undergo it every 7-10 days. You should choose a rational way of delivery (decide on the planned procedure of a caesarian section if there is a cicatrix on the uterus or the baby is too big).
Keeping the condition of the baby and the condition of the cicatrix on the uterus under control (cardiotocography, an ultrasound investigation of the uterus – the focus is the area of the post-operation cicatrix). A diagnostics and detection of the possible uterine rupture or the uterine rupture that has already started.