Pregnancy And Intrauterine Device (IUD)
Contents:
- What to Do if You Get Pregnant With Your Intrauterine Device
- Pregnancy Symptoms
- Additional Measures to Birth Control Methods
- What to Do if You Have IUD Pregnancy
What to Do if You Get Pregnant With Your Intrauterine Device
Unfortunately, any woman may get pregnant even if she has an intrauterine device implanted in her uterine cavity. This happens in spite of the fact that intrauterine systems are known for very high Pearl Index to prove this birth control method (it means, that "faults" are too rare). Let's discuss the symptoms of IUD pregnancy, the ways to identify the fetus development beyond the uterus (that is life-threatening) and what to do if the pregnancy exists and whether it is possible to save pregnancy?
Pregnancy Symptoms
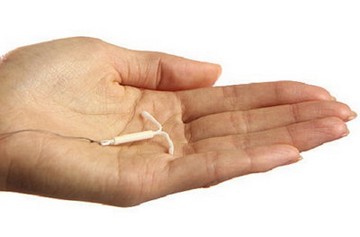
When the intrauterine device (IUD) is inserted into the uterus, a woman experiences no changes in her body as compared with administration of oral contraceptives (hormonal tabs). The ovulation is not blocked, endometrium keeps growing with regular periods. Sometimes periods may be heavier than those in women who use other birth control measures. So, is it possible to get pregnant with IUD? Yes! That's possible. The IUD merely blocks the way to the uterus and does not allow the fertilized ovum to impregnate into the uterus wall. However, this protection might weaken in some particular cases.
Late periods is one of the major symptoms of possible pregnancy. If such, the pregnancy test and/or blood check for HCG is recommended. Note that tests should be done in the first days of missed periods. Why is it so important? The point is that the ectopic pregnancy that occurs with IUD has the similar symptoms. Moreover, this is ectopic pregnancy that frequently occurs with IUD, especially in cases when there are synechias in fallopian tubes. By the way, the fertilized ovum may start developing in the cervix area not only in fallopian tubes. Both cases are life-threatening.
There may be other symptoms of pregnancy but they are not distinctive. These include the vaginal discharge in more intensive way, enlargement and tenderness in mammary glands, nausea, vomiting and slight rise of body temperature.
Additional Measures to Birth Control Methods
No, we are not going to talk on how to withdraw or about chemical birth control means like vaginal suppositories or tabs. Each female with IUD should be aware of several simple rules to follow.
- To see the gynecologist every year and have the ultrasound scan of the uterus. Doing that, it is easy to find out if the IUD shifts or it is wholly out that is risky for unplanned pregnancy. The rate of IUD pregnancy is about 3 %. That means that this birth control method fails in 3 out of 100 females.
- To check the length of IUD strands that go out from the cervix on your own. If they are longer than they were originally, it might tell about the shift of IUD into the cervix. Their absence may be the sign on the IUD falling out, all beyond the control of a woman, for example, during hygienic procedures. In this case, an extraordinary ultrasound scan of the uterus is recommended. If the IUD shifts, it should be removed. If it falls out, the pregnancy test is performed.
- Each IUD has its expiry date. It is about 5 years upon which period it should be removed and, if required, to be replaced with the new one. If not, a female is at the risk to have the IUD grown into the uterus wall. That’s difficult to remove it then. Moreover, she is at the higher risk to get infected.
What to Do if You Have IUD Pregnancy
Any single female wonders what to do if IUD pregnancy would be her case. Is this life-threatening? Is this dangerous? Specifically, it’s only you who take the decision on saving pregnancy or abortion. If it is decided to be removed, both the fetus and the IUD will be removed, if the device is still in the uterus.
However, it’s feasible to save the pregnancy in some cases. The risk of healthy pregnancy is at the doctor’s competence and qualification to identify. In some cases, the doctors advise that a woman waits until her delivery date to remove the IUD out of the uterus, providing that the IUD does not prevent healthy development of the fetus as could be visualized by the ultrasonography. A common IUD (non-hormonal) does not result in fetus malformation. A good pregnancy and IUD may co-exist.
If IUD is hormone-based, it should be removed for sure. Such devices release hormone into the uterus cavity to some extent that might penetrate the placenta to affect the fetus through the blood stream. This is quite dangerous. In this case, removal of the IUD might result in miscarriage. By the way, there is also the risk of miscarriage and various infections with the IUD not removed in pregnancy. Such pregnancy should be carefully monitored with more frequent ultrasonography and measure taken to prevent the miscarriage.